Afghanistan: “Everything went so fast”
In the bitterly cold Afghan winter, lower-income families face unexpected risks as they struggle to keep warm. Doctors Without Borders/Médecins Sans Frontières (MSF) nurse Diana Pereira de Sousa shares the story from Kunduz, a city in northern Afghanistan …
“Can you come to the ER? It’s urgent.” The call was from Boyd, one of our doctors. When I got there I saw some of our senior medics talking fast. Five burns patients had been rushed to the ER.
I had no idea what would come next.
In the red zone there was a woman and four young children, all of them with second and third-degree burns. The red zone is where we treat patients in critical, life-threatening conditions.
Assessing the patients, it was difficult to understand how extensive the injuries were, the percentage of the body surface burned. This was not like the burns we’d seen before – when a toddler spills hot water, for example. Although we admitted patients with burns related to trauma, the complexity and severity of these burns required a higher level of care than we could offer.
Another three patients arrived, also with severe burns. A man, a pregnant woman, and a 10-year-old-child, unconscious.
We decided to admit the woman and three of the children. The child in the most critical condition would be referred to the Kunduz Regional hospital, as he was at risk of losing his airway and we did not have the capacity to ventilate patients.
As we were sharing the plan with the ER team, another three patients arrived, also with severe burns. A man, a pregnant woman, and a 10-year-old-child, unconscious.
As the new arrivals were rapidly assessed, the confusion was clear on all of our faces. What had happened? And crucially, were there more patients coming?
Still unsure if we were dealing with a mass casualty incident like a bombing, we learned that referral to the regional hospital was not an option. The last three patients had been sent from there: they did not have capacity to treat them.

“Do you know what the most frightening thing is? Being in a resuscitation room with five children … and none of them crying.”
Everything went so fast. In a few minutes we had all the patients on IV fluids and the first set of observations done. Around me the red zone was full of people. We needed to make decisions, quickly.
Together, we came up with a plan.
Every department in the hospital adapted to give these patients the best possible chance of survival. The list for the operating room was cleared of all non-emergencies, patients who could be safely discharged were moved from the intensive care unit (ICU) and inpatient department to provide beds.
Do you know what the most frightening thing is? Being in a resuscitation room with five children, four of them awake, with 30 to 50 per cent of their bodies burned, and none of them crying.
I could hear the staff talking. I could hear the rustling of the foil survival blankets. But I could not hear the patients themselves. Very few people like to hear a child cry, but in a hospital it can tell us a lot about their condition.
Without proper treatment the body can start to shut down.
Involuntarily immobilized by the burns covered with thick gauze, our patients were also not moving. Their stillness and silence was heavy in the room.
Automatic mode
In medicine, sometimes you go into ‘automatic’ mode. I think we all did that day. In a fast but smooth way the patients were given the best treatment we could with the knowledge and resources we had at that moment.

When someone is severely burned there is an inflammatory response throughout their body to try compensate for the damage. One of the consequences is patients continuously lose fluids from the burns, which can lead to severe dehydration and electrolyte imbalance. Without proper treatment the body can start to shut down.
It was magnificent to watch the team adjust with such speed and dedication.
Our ICU was transformed in a burn unit, where six of the patients were admitted for close monitoring, aggressive fluid therapy and pain management.
Burns patients are at heightened risk of infections, so the ICU team (cleaner, nurses and even doctors) assisted in deep cleaning the unit even more thoroughly than normal, and adopting the use of personal protective equipment, such as gown, gloves, and face masks. It was magnificent to watch the team adjust with such speed and dedication.
The explosion
We desperately wanted to talk with the patients and their family members, but they only spoke Uzbek, which meant very limited numbers of staff could communicate with them.
Eventually, we learned what had happened. The family had gone to the home of a relative to offer their condolences after a burial ceremony. It was so cold that the gas cylinder froze, so they brought it into the house and placed it near a small heater to thaw.
They described what happened with tears in their eyes.
Some of the children were sleeping when the gas cylinder exploded, but they managed to get everyone out before the entire ceiling collapsed. One of the family had a video of the destroyed house. They described what happened with tears in their eyes.
Very sadly, the severity of his burns meant that the oldest child, a little boy of around 10 years old, passed away less than 36 hours after he was admitted.
Keeping faith
Despite the loss of their young patient, our team kept faith. They worked incredibly hard to care for the other burns patients, including the little boy’s father and two sisters.
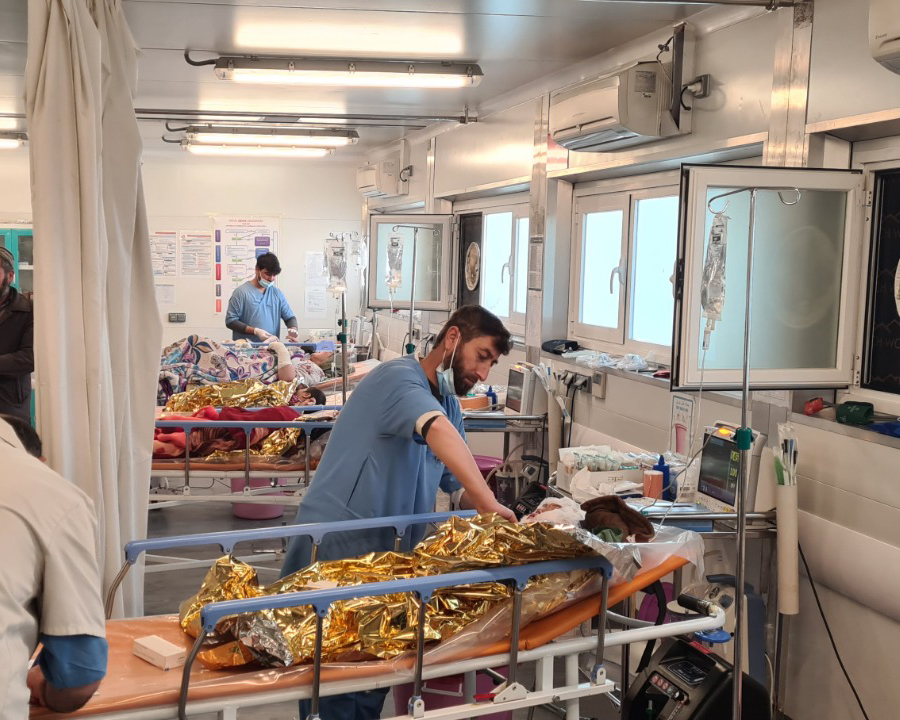
Making space for play
As the weeks went by, we could see the complexity and prolonged hospitalization that family would face. Every week each of them would have two or three surgeries to remove the dead tissue and prevent infection.
It is very difficult to see children who do not smile, so as the children gradually became stronger, the ICU team took it as a challenge to make them feel safe and able to play. We used music, cartoons, and dolls made by inflating surgical gloves like balloons. One day we realized they had stayed almost two months in the ICU without seeing the sky, so we found a way to take them outside for contact with fresh air and nature.
Three months on
Three months after their admission, four of the family were well enough to be discharged. I won’t forget the two little boys, Abdul* and Abbas, waving to me when they returned to the hospital to have their dressings changed. Seeing them walk and smile, like typical children, was so rewarding and made me hopeful for the two little girls who were still in hospital.
One of thing I remember most was the first time Abdul laughed.
At that point the girls’ father was transferred to a burns unit in Kabul, and the girls, Sima and Habiba, were well enough to leave the ICU and be treated on the inpatient ward.
Looking back, it is not easy to put into words how I feel about these patients. One of thing I remember most was the first time Abdul laughed. It was two weeks after they were first admitted. Gradually we helped the children feel comfortable and built trust. One day, one of the nurses tried gently tickling Abbas, and was rewarded with a shy smile. She tickled Abdul, and we got the first genuine laugh we had heard.
Suddenly the team was contagious with laughter and that moment gave us a boost of energy that everyone needs to keep up hard work. Those two weeks had been intense and uncertain, but hearing Abdul laugh, I felt that my chest was not big enough to hold all that joy.
*All names changed












