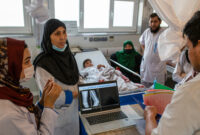
‘It was the first time I had seen someone in person so viscerally affected by war’: Care amid conflict in Afghanistan
For almost two decades, active conflict has made life extremely difficult for people in Afghanistan. In addition to those who have been directly impacted by violence, many others can’t even access basic healthcare. Hazards such as landmines, bombs, active fighting and the danger of being caught in crossfire can make simply travelling to or from a hospital a dangerous undertaking.
Jesse Perry, a Vancouver nurse, was confronted with the human impact of Afghanistan’s ongoing conflict during his recent assignment with Doctors Without Borders/Médecins Sans Frontières (MSF) in the country’s Helmand province. He remembers being present in the maternity ward at the MSF-supported Boost hospital in Lashkar Gah when a patient learned that an airstrike in her home village had killed her two older children.
“It was the first time I had seen someone in person so deeply, viscerally affected by this war that has been going on for most of my life,” he recalls. “I looked at this mother and I did not know what to say to her. I looked at her newborn child who continued to need supplementary oxygen and antibiotics. I was in the awkward position of trying to convince this mother either to stay here or leave her child with us, so that she could hitch a ride to travel at least three hours through military checkpoints and illegal roadblocks to bury her children.”

‘When they arrive, they are already in bad shape’
The woman’s circumstances were deeply tragic, but unfortunately not unique. In Lashkar Gah, MSF teams often see patients who have travelled long distances and for hours to reach the hospital. “They are delayed by checkpoints and insecurity on the road, so they often arrive late and in a critical condition,” says Mia Hejdenberg, a former MSF head of mission in Afghanistan. “When they eventually reach us, many have to interrupt their treatment to return home when they feel safer.”
This can be a particularly difficult challenge for pregnant women. Over a nine-month period last year, 13,208 women were admitted to the Boost hospital’s maternity ward, including 5,218 for complicated deliveries. ‘’Many patients come here already in shock after a post-partum bleeding because they delivered at home,” says Rita Alexandra Batista Luz Mano, an MSF gynecologist. “When they arrive they are already in bad shape, and it’s very difficult to recover from that. This month we had five women who died upon arrival.”
A lifeline in a region lacking in quality medical care
But without the Boost hospital many more would be at risk. It is the only referral hospital in Helmand province, and serves approximately one million people. MSF supports all the hospital’s departments, including emergency, surgery, maternity, pediatrics and internal medicine.
At the end of 2019, MSF commemorated 10 years of providing care to patients at the Boost hospital. In 2009, five years after withdrawing from Afghanistan following the murder of MSF staff members in Badghis, the organization resumed operations in the country, prompted by a deteriorating humanitarian situation and an increasing lack of civilian healthcare. Southern Helmand province was one of the areas most affected by conflict at that time, and the project in Lashkar Gah was the second MSF project to open in the country. The aim was to revitalize the hospital and deliver quality and free-of-charge healthcare to the people of Helmand province.

‘We are seeing thousands of patients every month’
“When MSF arrived at Boost hospital in 2009, the hospital had 150 beds with about 20 patients,” says Marcella Kraaij, former MSF project coordinator in Helmand province. “Now we have around 400 beds and more than 900 staff, and we are seeing thousands of patients every month. I think that the biggest difference between Boost hospital in 2009 and 2019 is the consistency and availability of resources, in every sense of the word. The buildings have been improved, the number of staff has been increased, a lot of trainings have been provided to the staff, and supplies are always available.”
Last year, MSF’s activities at the hospital increased in almost all the departments. Bed occupancy is often at 100% and the number of admitted patients is 30 times what it was a decade ago, growing from around 120 per month in 2009 to an average of 3,500 per month in 2019.

But even for those who have been able to access essential medical care within the hospital’s walls, Afghanistan’s ongoing conflict continues to cause tragedy and hardship. Jesse Perry is now back home in Vancouver, but he still vividly remembers the young mother who needed to travel home to bury her children, even as her newborn son had to remain and receive care at the only health facility available.
“What could I possibly have done to help her?” he asks. The answer that he and his MSF colleagues found was to continue providing care where it was needed most. “We could continue treating her baby,” he says. “And making sure he was fed until she returned.”

rong>

rong>