Cascading global crises: A call for a radically inclusive, equitable and innovative response
COVID-19, Climate Crisis & systemic inequality
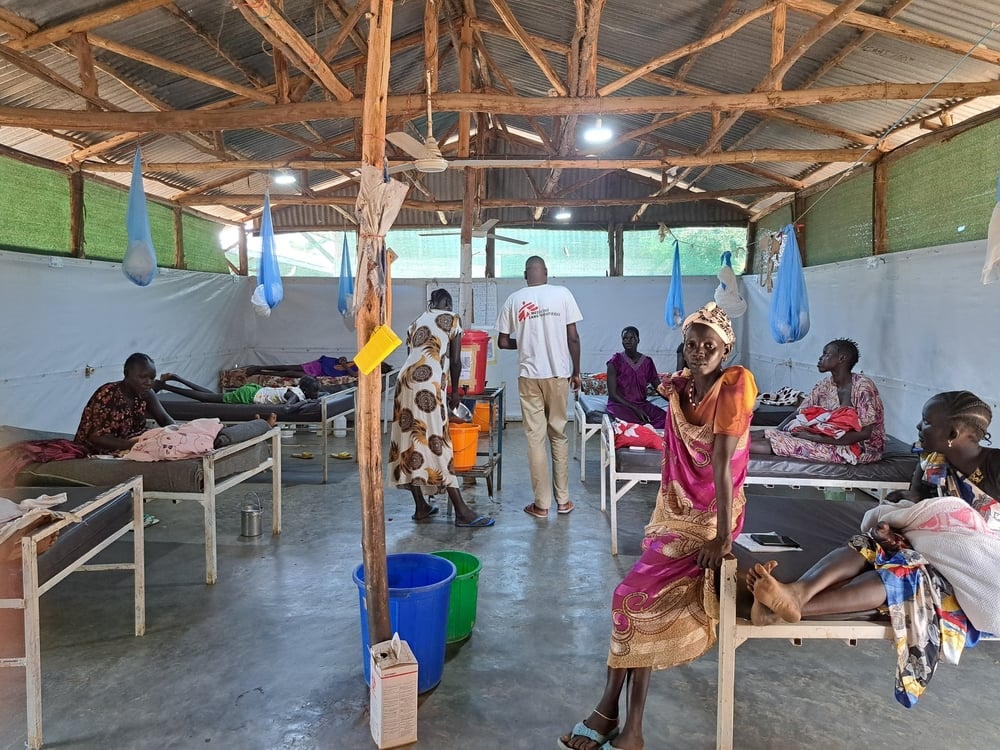
COVID-19 continues to affect millions and distress healthcare and social services, the ongoing humanitarian response and the global economy. In many places where MSF works, such as in Yemen, COVID-19 is bringing already-fragile health systems to their knees. A devastating pattern everywhere that Doctors Without Borders/Médecins Sans Frontières (MSF) sees too is the new coronavirus is hitting marginalized and excluded peoples the hardest.
By Nora Dettmer, Advocacy Project Manager, MSF Germany and Carol Devine, Humanitarian Affairs Advisor MSF Canada and Lead, Climate-Smart MSF Transformational Investment Capacity project.
The pandemic also dovetails with the global protests against systemic racism and violence that first erupted in the U.S. on May 26, 2020, after George Floyd was killed by the police and also in response to other cases of recent and historic structural violence. In the U.S., where MSF operates for the first time ever, Black and Hispanic/Latino groups are dying disproportionately from COVID-19[1] and already face health disparities.

If that’s not enough, a recent report cites May 2020 tying with May 2016 as the earth’s warmest May on record and 2020 is on track to be one of the five warmest years in recorded human history.[2] Warmer temperatures play a role in disease outbreaks, extreme weather events, food and water insecurity, wildfires and more and will bring heightened effects including on COVID-19.
While there is no direct connection between the emergence or transmission of the new coronavirus and climate change[3], the outbreak highlights how climate change compounds health effects, especially for already-marginalized populations. Science shows that COVID-19 has a zoonotic origin.[4] Zoonosis – transmission of disease from animal to humans, is the highest new infectious disease burden today[5] and our human disruption of nature plays a part. We’ve encroached on wildlife, deforested and destroyed their habitats, and illegally trafficked them, resulting in a spillover of pathogens. Landscape changes are linked with the emergence and re-emergence of diseases. As well, biodiversity loss is a risk multiplier for infectious diseases. [6]
This blog will explore effect multipliers and lessons being learned from COVID-19 including MSF’s rapid adaptation and innovation, with a frank look at systemic inequality, as well as at common needs for equally accessible, sustainable healthcare and humanitarian responses.
“COVID-19 is not a black swan event,” said Aarathi Krishnan, Humanitarian Futures and Strategic Foresight Advisor, at the recent MSF Scientific Days UK panel on Stretching the Frontiers of Humanitarian Thinking. We were forewarned. If Ebola was the bellwether for COVID-19, what does COVID-19 forewarn? We also knew about structural, social and economic inequality that makes certain people and groups more at risk of health problems. COVID-19 is yet another revealer of systemic racism.
MSF is responding to COVID-19 around the world in some 70 countries, in addition to existing programs. We are not only seeing inequalities between countries but also within countries, including the planet’s richest economies. Racism often works in conjunction with economic exploitation and exclusion, which forces individuals to work under precarious working conditions, resulting in more exposure to COVID-19 (or indeed many other diseases).
Today, the epicentre is Latin America. In Brazil, the most impacted people are those facing deep structural inequalities, including refugees from Venezuela. “Despite its relatively small population, the state of Amazonas is among the regions with the highest absolute number of deaths by the new coronavirus in Brazil,” says MSF in late May 2020. Manaus, in the heart of the Amazon, is a hard-hit region also with a record number of fires and unprecedented deforestation.
Bangladesh’s perfect storm: Addressing the climate and COVID-19 emergencies simultaneously
COVID-19 exposes the deep inequalities that affect people’s capacity to respond to crises, no matter whether it is a dengue outbreak or a cyclone. People living in Bangladesh face both. Financial and healthcare supports and resources for some are not the only prerequisites for societies to recover – as we see in Europe and Canada, for example. The consequences of social and economic inequality are undeniable, and starkly so in Bangladesh.
MSF’s experience in Kamrangirchar suggests that land pressure and increasingly poor farming yields are key drivers of migration to this urban slum of Bangladesh’s capital, Dhaka, where slum-dwellers are exposed to highly polluted living environments and hazardous working conditions. Air pollution, a major cause of non-communicable disease, kills an estimated seven million people a year; it’s worsened by increasing CO2 emissions. A Harvard study shows that COVID-19 mortality increases where there are more carbon emissions.[7] But there’s more: air pollution and COVID-19 race data still represent a small sample but found that people with more exposure to air pollution are 15 per cent at higher risk of mortality, and African Americans and poorer communities are more exposed to air pollution.[8]
Also, Bangladesh hosts the largest refugee camp in the world, Cox’s Bazar. Rohingya refugees are stuck in cramped, squalid shelters with up to 10 family members to a room – making social distancing impossible. They are not only vulnerable to infectious diseases but also the possible devastating impacts of tropical cyclones; the most recent, Amphan[9], didn’t hit Cox’s Bazar but drove millions into evacuation. Evacuation is difficult even when shelters are available, but during a pandemic, shelters cannot be used at full capacity and already Cox’s Bazar has an inadequate number of shelters. This leaves refugees and local populations exposed to a double threat.
Being trapped and unable to move is difficult for anyone but can be extremely dangerous and even deadly for certain groups, such as women in closed spaces and isolation. Evidence suggests that climate-induced crises[10] and the current COVID-19 outbreak[11] increase the risk of domestic or intimate partner violence.
Health for everyone
COVID-19 is far from over. The concept of global health security only works if we pay the same attention to the outbreak in Bangladesh as we do in Italy. We should ask ourselves: Security for whom and from what? It is extremely worrying to see that many states’ response to marginalized communities struggling with COVID-19 infections has been fences and unwarranted collective isolation, destroying trust and access to health services and ultimately jeopardizing an effective response. Global health security does not mean health for the privileged few and closed borders to everyone else. We have seen it with Ebola and need to learn from it. Wealthy nations will fund and prioritize what threatens them, which is why we suddenly see so much happening that seemed impossible a few months ago: wealthy nations especially, rapidly reducing our carbon footprint – a huge challenge; pulling out all the stops to develop a vaccine in record time – unthinkable when it comes to diseases such as multidrug-resistant tuberculosis (MDR-TB) that disproportionately affects marginalized and racialized communities. It is yet another example of why we cannot talk about COVID-19 or the climate crisis without confronting the structural inequality that lies at the centre and ultimately influences our response. Global health security must mean health for health’s sake, for everyone. No exceptions.
This cannot continue to be us versus them. Tackling a pandemic and the climate crisis demands an integrated response, a multi-hazard approach that involves and includes everyone. This also means we need to listen to affected communities, to local actors, build trust and collaborate, particularly amidst an increasing environment of misinformation, fear and xenophobia. We need to also voice the urgency for mitigation of climate impacts and to dismantle systemic racism in our work.
A word on smarter travel, sustainability, waste and equity
COVID-19 border closures and global lockdowns have had a deleterious impact on people and on MSF’s operations. MSF and others struggled to have enough PPE for healthcare workers and patients. We grappled with supply disruption and travel restrictions but also collaborated and found solutions. Amidst this, we adapted and helped many in need.

A destructive pandemic, especially for the poorest and most marginalized people, is the worst way to force carbon emission reductions. Despite the devastation, studies show a temporary if significant reduction in air pollution and greenhouse gases[12], and the health benefits and avoided deaths related to improved air quality.[13] The flight bans disrupted so much but also gave a temporary ’cease-fire’ from harmful carbon emissions and showed us nature’s resilience and our ability to adapt. But without urgent actions, global CO2 levels will continue to climb and thus exacerbate health and humanitarian needs.
MSF has already committed at the associative and operational levels as well as in ad hoc actions to reduce our environmental impact and here COVID-19 forces us to adapt in the transformational way we aspire to but weren’t able to do so quickly. How to capture and retain and leverage lessons from the massive disruption to our way of working? We’ve largely adapted to non-essential travel by leveraging virtual platforms to hold meetings etc. COVID-19 also exposes inequities in access to internet and remote-work capability and this must be tackled. Internet access and social protection are necessary for coping and recovery, especially for those excluded and displaced or stateless peoples at significant additional risk.
COVID-19 also highlighted the serious energy needs for the health response in pandemics and in general – for autonomous, affordable, accessible energy for ventilators, oxygen, air conditioning for pharmacies, hospitals and clinics and cold chain etc., and for when there is a hopeful vaccine.
MSF is making strides in reducing our negative environmental impact and increasing cost efficiencies through accelerating solar and renewables use, reducing air freight, conducting travel efficiency studies and doing more measuring and mitigating of negative impacts. All efforts are rightly focused on containing the outbreak and responding to COVID-19 and heightened humanitarian needs. But we understand that little if any attention is paid during this pandemic by MSF and others to the environmental and social impact of production and waste from COVID-19.
Let’s scale up these efforts at reducing our negative impact and including sustainability in our work as an inherent part of a more planet- and patient-friendly and climate-resilient humanitarian response. There is no vaccine for the climate crisis.
‘Do no harm’ in our operations is not a bonus, it’s necessary part of our work. Moving towards Equity Diversity and Inclusion (EDI) is also no longer aspirational, it’s paramount to achieving MSF’s medical objectives, and fulfilling our duty of care to patients, staff and the populations we aim to serve. These cascading crises give pause to take a serious look at our internal organizational structures, policies and ways of working that perpetuate any of the colonial and oppressive roots in humanitarian aid.
The way forward
The closer we look, the more we realize this is like a Matryoshka Russian doll of crises, which can be overwhelming. But the concurrence or convergence of COVID-19 and the climate crisis, despite their destructive forces, also highlights common solutions for MSF and the world. We must do what we can from a health equity, adaptation, mitigation and leadership place to ensure healthcare and humanitarian systems are more prepared, inclusive and resilient.
The pandemic has also shown MSF, as from its beginnings, we are lateral thinkers and doers and are innovating fast – solutions are closer to the critical points we cannot access, closer to the strength of independent local action and collaboration with communities and the even-wider potential of telemedicine.
In addition to our work, which has at its base the belief in equality and healthcare for all, we need to actively adopt an anti-racism and anti-exclusion strategy to fight COVID-19 and other health exclusions and to ensure we do not pollute and that we do no harm in our response.
MSF has been advocating for access to personal protective equipment (PPE) and basic health services for all, for the inclusion of refugees and migrants in public health responses and respect for international law, as well as for vaccines and diagnostic tests to be accessible and affordable for all. We are also speaking more internally and externally on wider public health crises only intensified by COVID-19 and the climate crisis, and stating this with a unified voice would even be stronger.
We need to walk the talk and make sure we don’t become performative allies – this also means reflecting on our own biases, those of us with privilege, and what we can concretely do to tackle them. We are part of a deeply unequal system and it is our responsibility to be a part of changing it. That means those of us like us, checking our own (white, western) privilege and bias that contribute to the inequality that we are trying to fight. No matter how open-minded or accepting we believe ourselves to be the fact remains we all carry prejudice and bias whether we like to hear that or not – it influences our work and modus operandi. We need to be radically inclusive and operate differently, building on what is working – now almost five decades of pragmatic adaption and impact – and changing what isn’t, starting yesterday.
REFERENCES
[1] CDC report on COVID-19 effects on racial and ethnic minorities
[3] https://www.who.int/news-room/q-a-detail/q-a-on-climate-change-and-covid-19
[5] https://www.cdc.gov/onehealth/basics/zoonotic-diseases.html
[6] https://www.ipcc.ch/site/assets/uploads/2018/02/WGIIAR5-Chap19_FINAL.pdf
[8] https://www.unenvironment.org/news-and-stories/story/air-pollution-hurts-poorest-most
[9] https://www.bbc.com/news/world-asia-52734259
[10] https://unfccc.int/news/climate-change-increases-the-risk-of-violence-against-women
[12] https://www.nature.com/articles/s41558-020-0797-x https://www.thedailystar.net/opinion/politics-climate-change/news/covid-19-and-climate-change-1885357
[13] https://www.thelancet.com/journals/lanplh/article/PIIS2542-5196(20)30107-8/fulltext