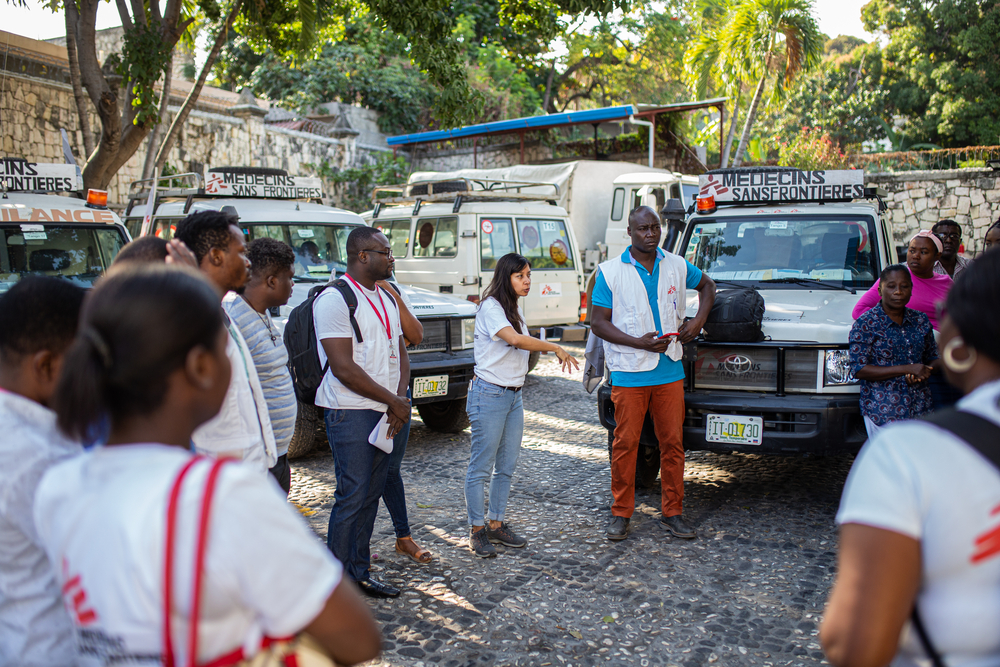Haiti: MSF mobile clinics in Port-au-Prince treat people stranded by violence
Vulnerable people in Haiti’s capital of Port-au-Prince are caught in a spiral of ongoing violence and insecurity, living under the threat of stray bullets and kidnappings as well as economic precarity. Doctors without Borders/Médecins Sans Frontières (MSF) runs mobile clinics almost daily to treat hundreds of children, women, men, and elderly people trapped in their neighbourhoods. In the first four months of 2023, MSF mobile teams have treated a total of 7,781 patients and have distributed more than 300,000 litres of drinking water in the areas of Delmas, Bel- Air, and Bas Bel -Air, where people have been particularly affected by violence. Another 300,000 litres of drinking water and 607 hygiene kits have been distributed to the population displaced by violence in the neighborhoods of Fort National and Poste Marchand in the month of February.
A humanitarian crisis
A series of major political, social and economic events, have resulted in a complex, multidimensional humanitarian crisis. Access to essential services, including healthcare and mental health care, water and sanitation (WASH), is severely compromised across Port-au-Prince, and especially in the most violence-affected neighborhoods. Conflict between rival armed groups makes it difficult for people to move freely across the city, and much of the population live in extreme precariousness.

© Alexandre Marcou/MSF
MSF health promoters provide patients with information in front of the building where the pharmacy, maternity and doctor’s consultations are located. Haiti, 2023.
The role of mobile clinics
At least four times a week, three MSF cars transport a multidisciplinary team composed of doctors, nurses, psychologists, health promoters, midwives, and water specialists, as well as medical material to treat patients in areas affected by urban violence in the centre of Port-au-Prince.
“Mobile clinics are necessary in a context like Port-au-Prince” explains Michele Trainiti, MSF country director in Haiti. “Health facilities in some of the most violence-affected neighbourhoods are closed. Partly functioning health structures are difficult to reach and unaffordable for many. People are too afraid to travel due to violence and insecurity, including the high risks of stray bullets, and even then, transportation options are limited. In addition, public healthcare facilities often face regular shortages of staff, medicines and supplies – so even when people are able to overcome all the barriers to reach a health centre, they may not be able to receive the care they need. “Although not perfect, mobile clinics are flexible and adaptable. They allow us to bring healthcare closer to patients in parts of the city affected by violence. We can therefore overcome some of the barriers that people face in accessing healthcare,” adds Trainiti.
Addressing mental health, sexual health, and other issues
The violence people experience, and witness have a significant impact on their mental health, according to Camille Dormetus, MSF psychologist at the mobile clinic, “the sound of bullets, the fear of being attacked by armed groups, the death of relatives… are parts of the traumatic situation experienced by our patients. I saw many patients suffering from anxiety, depression, with sleep disorders or hypervigilance… with some of them consuming psychoactive substances to escape from their reality.”
Dr. Engleed Emeran also works with the mobile clinic team. “I usually see around 50 to 70 patients on a normal day, mostly young women for sexually transmitted infections, old women for chronic pain and hypertension, and young children with respiratory infections” explains Dr. Emeran. “The challenge with mobile clinics is that we cannot conduct more advanced diagnostic methods, but it is the only way for many people to access free health care and medicines” she concludes. The needs are so dire that even the provision of the most basic needs is essential.
At another part of the clinic a medical team treats numerous cases of scabies, the most common morbidity seen in all clinics. Scabies is a contagious skin condition caused by tiny mites that burrow into the skin and is a symptom of unsanitary living conditions. It is especially common in parts of the city where access to water is limited, and sanitation facilities are inadequate. “Through our mobile clinics, we provide primary healthcare along with health education, and refer patients with more complicated cases to other health structures. We also provide drinking water and repair sanitation facilities where these services are existing. We are always looking at what additional assistance we can provide, but the needs are just too massive.” concludes Michele Trainiti.
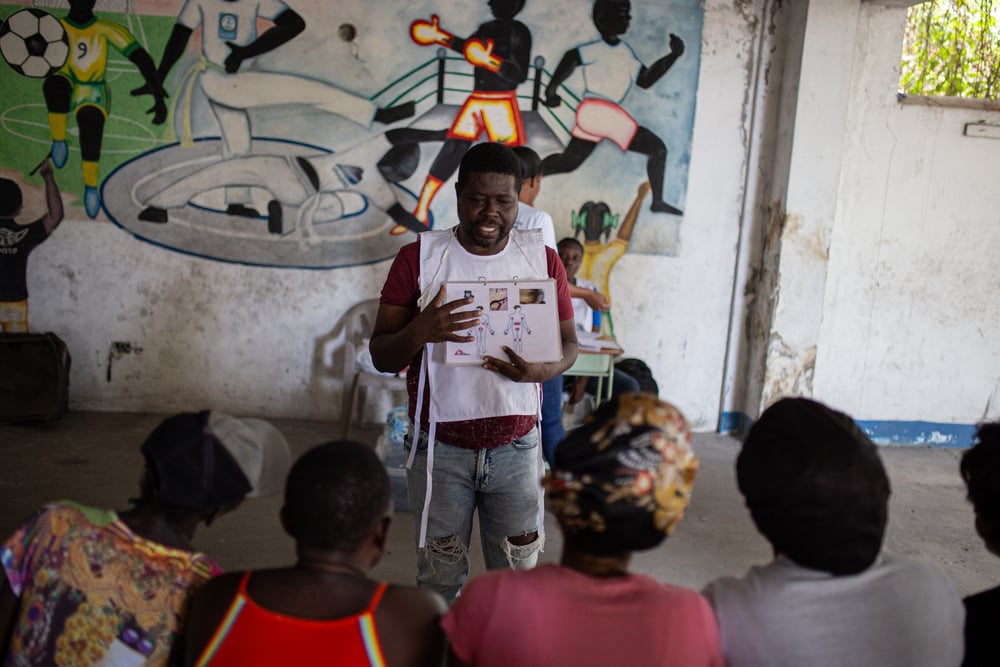
© Alexandre Marcou/MSF
A health promoter explains how people can contract scabies, how to heal from the infection and avoid contagion. Haiti, 2023.
Adapting to changing needs
MSF’s mobile clinics were suspended from September to December 2022, partly due to the Peyi Lòk (mass protests) and partly due to the cholera outbreak that gripped the country. At the onset of the cholera outbreak the mobile clinic teams were redeployed to respond to it, setting up new treatment facilities and other community-based outbreak response measures. MSF treated more than 16,829 patients in collaboration with the Haitian authorities between October 2022 and April 2023. Although the mobile clinics are up and running again, they are doing so at a moment in which levels of violence are extremely high, making continued flexibility a priority.
MSF has been working in Haiti for 30 years, providing free quality medical care for all the Haitian people, and it remains committed in its support. In 2022, our mobile teams carried out 17,800 consultations.