Home | What we do | Advocacy
Beyond the Headlines: A Canadian’s Testimony from the Central African Republic
By Jason Nickerson, Doctors Without Borders/Médecins Sans Frontières (MSF)’s Humanitarian Representative to Canada.
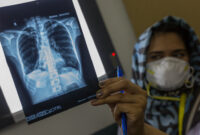
Earlier this year, violent clashes erupted in Ippy, an area located in the centre of Central African Republic, forcing thousands of people from rural villages to flee to Ippy town and the camps for internally displaced people that were established around it. MSF sent an emergency team to respond to the emergency, providing medical care and installing water and sanitation infrastructure like water points and latrines.
This emergency, like many others in places where MSF works, takes place far from the attention of international media, even as armed violence continues to rage in many parts of Central African Republic and other countries. Yet the crisis in CAR, one of the world’s poorest countries, is predicted to get worse, leaving more than 60% of the country’s population in need of protection and humanitarian assistance this year – a level of need not seen in five years.
International support is vital
The country depends almost entirely on international assistance for healthcare, and an ongoing civil conflict between government forces and armed groups, combined with nearly non-existent levels of infrastructure and state services, have left CAR’s population experiencing some of the worst health indicators in the world. At the same time, the world’s attention is elsewhere. The reasons for this are multi-faceted, but the impact is clear: access to healthcare for many people in Central African Republic is out of reach.
…the crisis in CAR, one of the world’s poorest countries, is predicted to get worse.
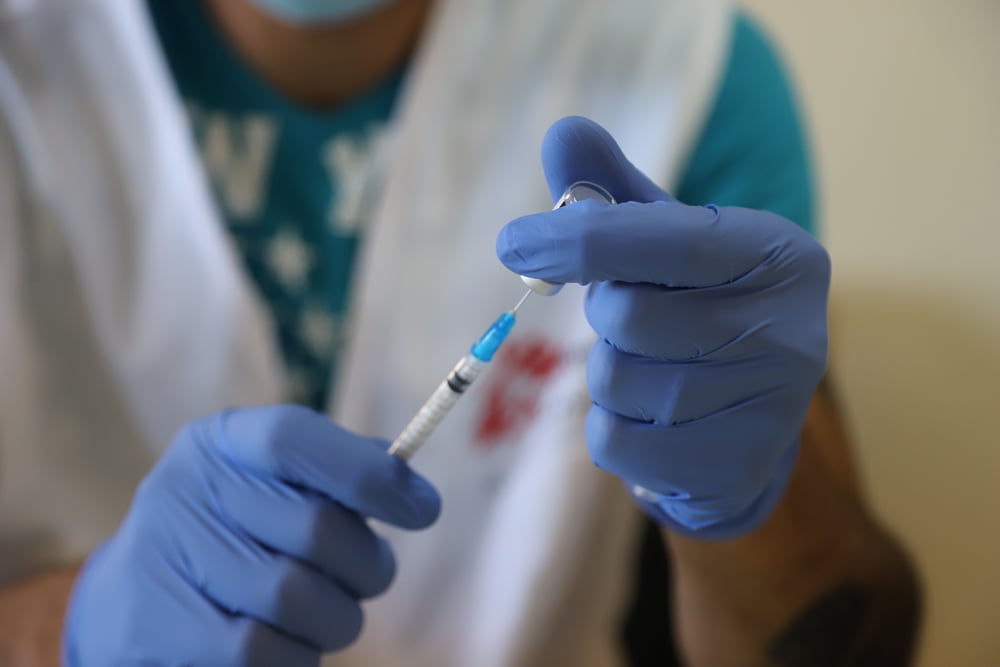
In March and April of this year, I was on assignment in CAR, working with our teams to recharge our advocacy on this emergency, including our medical work in areas such as HIV, malaria, and sexual and reproductive health – there are challenging gaps in access to each of these services for people throughout the country. In speaking with colleagues and with people in the communities where we work, the spectrum of challenges that people are working to overcome are clear. For example, life in rural parts of the country means navigating often treacherous and dangerous roads (due to poor road conditions, but also the presence of armed groups) to reach healthcare that simply does not exist in many parts of the country. These challenges aren’t easily fixed, as they implicate almost every aspect of the building blocks needed to run a functional health system, and it takes time to strengthen them and build them up. Meanwhile, humanitarian organizations like MSF continue to be needed to provide emergency access to lifesaving care.

Shortage of healthcare workers
A shortage of health workers, for example, is regularly highlighted as a major impediment to scaling-up quality care in CAR. The country lacks significant numbers of qualified personnel: There are only 0.1 physicians per 1,000 people and 0.206 nurses and midwives per 1,000 people. This roughly translates into approximately 350 physicians and 995 nurses and midwives for the entire country of 4.8 million people. Compare this to Canada, which has 2.4 physicians per 1,000 people and 11.8 nurses and midwives per 1,000 people, and is still facing significant and growing impediments to providing healthcare as a result of not having enough qualified health human resources, and you start to get a sense of the scale of the challenges. Health professionals don’t appear overnight; training a physician can take 7 years, training a nurse can take 4 years.
Despite these challenges, some progress has been made. CAR, which has one of the lowest rates of antiretroviral therapy coverage for people living with HIV in the world, has increased this coverage from 28% in 2015 to 58% in 2020 – far too many people are still being left behind, but the progress is impressive. More is being done to close this gap.
There’s clearly a disconnect between what makes it to the top of the news headlines and what’s having a major impact on people’s lives around the world, and at a time when the world’s attention is focused on the seemingly never-ending COVID-19 pandemic, and now the war in Ukraine, crises in Central African Republic, South Sudan, the Rohingya camps in Bangladesh, and elsewhere are falling off the radar. While we can’t reasonably expect everyone to follow every crisis, I think we should expect more – more media coverage of neglected crises, more humanitarian assistance provided on the basis of need, and all-around more attention being paid to responding to people’s urgent needs.