The Last of Drugs: Making sure important medicines are still there when they’re needed
By Adam Houston, Medical Policy and Advocacy Officer for MSF Canada
One clear lesson from the popular post-apocalyptic television drama The Last of Us is that it is far more enjoyable to vicariously watch a pandemic unfold on TV than experience it yourself.
The show is having a cultural moment, including here in Canada where it was made; filmed in Alberta, it has been called the largest Canadian television production of all time. Its portrayal of a fungus that turns people into zombies – based on a real fungus that fortunately exerts its effects on insects, not humans – has in turn drawn more attention to the more serious topic of what might cause the next pandemic. In this vein, it has served as a reminder that fungi themselves can pose a serious public health threat; they even have pandemic potential, something aptly demonstrated by severe mortality in pandemics afflicting non-human animals like amphibians and bats around the world (including in Canada).
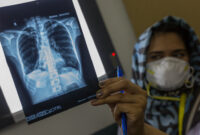
A preview of what such a pandemic might look like could be seen in the deadly surge of “black fungus” (mucormycosis) that occurred alongside COVID-19 in India, which claimed thousands of lives. The impact of this outbreak was exacerbated by drug shortages, with Doctors Without Borders/Médecins Sans Frontières (MSF) among those calling for better and more affordable access to treatment.
The need to ensure access to treatment during a major outbreak of a normally rare condition underscores some of the overlooked challenges in pandemic preparedness. In movies and on TV, responding to a pandemic often requires inventing a miraculous new cure for a novel pathogen. In real life, a response often also involves access to existing tools. Frequently given short shrift is the fact that access to some of these existing tools may be decreasing, or may not exist at all in some countries, meaning those tools are absent from the toolbox when they’re needed.
This is an issue facing many health systems, including Canada’s. Consider the tools available to tackle fungi. The World Health Organization’s Model List of Essential Medicines – the basic drugs that should be available in any functional health system – includes eight core antifungal drugs. Of these, only six are currently sold in Canada. It seems intuitive that one’s preparedness for a pandemic – hypothetical though it may be – is not optimal if one’s toolbox is missing 25% of the globally recognized basic tools.
Unfortunately, access to medicines in Canada, as elsewhere, is based on commercial interest; a drug that serves only a small number of patients under normal circumstances may vanish from the market, or never be brought to the domestic market in the first place, regardless of how important it is for those patients who do need it, or its potential utility under abnormal circumstances like a pandemic.
Market forces are clearly visible behind these two missing essential antifungals. Griseofulvin, an oral drug used to treat fungal skin infections when topical treatments prove ineffective, was available in Canada from multiple suppliers decades ago, but these all left the market in the late 1990s and early 2000s, rendering it unavailable. The other, flucytosine, has never been sold in Canada at all. This makes it particularly ironic that, during a recent period where there was only one supplier of flucytosine in the United States, that supplier – a Canadian company then known as Valeant – used its American monopoly to dramatically jack up the price of this old, off-patent drug, which itself was actually manufactured in Manitoba for export to the US. In turn, flucytosine is a drug one wants to have on hand when it is needed. For instance, it is one of three drugs found in current WHO treatment guidelines for the fungal infection cryptococcal meningitis, a co-infection of people with weakened immune systems that is the second-biggest killer of people with HIV worldwide. MSF continues to advocate for flucytosine to be affordable and accessible worldwide.
Antifungals are not the only example of a useful drug that may not be there when it is needed. For instance, in January 2023, the only supplier of the oral formulation of the antiviral drug ribavirin discontinued the product in Canada. This has serious consequences for a subgroup of hepatitis C patients who continue to need this medicine as part of their treatment. Ribavirin is also an important piece of the pandemic preparedness toolbox: It is one of the few drugs that exist to treat a range of hemorrhagic fevers. This includes hantavirus, a deadly disease found in Canada, and spread by rodent urine, droppings or saliva. It also includes both Lassa fever and Crimean–Congo hemorrhagic fever, two of the diseases prioritized by the WHO on its short list of Priority Pathogens with outbreak or pandemic potential, a list that also includes diseases like SARS, Ebola, and “Disease X”, the hypothetical, as-yet unknown pathogen that could cause the next pandemic. Like griseofulvin and flucytosine, ribavirin appears on the WHO Essential Medicines List, indicated for both hepatitis C and hemorrhagic fevers. It is not a wonder drug, but in the absence of superior alternatives, remains a vital tool to have in the toolbox to treat patients today, and be prepared for a pandemic tomorrow.
Entering a pandemic with important tools missing from the toolbox is not a hypothetical. Early in the COVID-19 pandemic, Canada faced a shortage of numerous drugs, both for drugs being used in the COVID-19 response and those used for other purposes. Factors driving shortages included increased usage in response to the pandemic, and the disruption of global supply chains. But in some cases, the pandemic was a sobering reminder that some important drugs simply were not available in Canada at all. Of the 30 drugs listed in Tier 3 Shortage – those shortages “that have the greatest potential impact on Canada’s drug supply and healthcare system”- in early June 2020, four, including three being used as part of the COVID-19 response, were no longer being sold in Canada at all. In the case of all four drugs, three of which are also on the WHO’s Essential Medicines list, the last remaining supplier had left the Canadian market before the pandemic. The failure to ensure important drugs remained available under normal circumstances meant they were no longer available precisely when they had the “greatest potential impact” on Canada’s healthcare system.
Many of the drugs discussed above, from flucytosine to ribavirin, are used by MSF in its operations around the world. Often, these operations take place in humanitarian settings where health resources are scarce. That these same medicines are wholly unavailable in a high-income, well-resourced country like Canada is an important reminder of gaps in pandemic preparedness. A pandemic is a global event, requiring a global response. As countries look at the role of access to medicines in a pandemic, both through international measures like the WHO Pandemic Accord currently under negotiation, and domestic measures like Canada’s new Biomanufacturing and Life Sciences Strategy, the focus is often on access to new tools, like COVID-19 vaccines.
It is important not to lose sight of the need to maintain access to the tools that already exist. Depending on the drug, approaches could range from beginning or maintaining local production, to improving international recognition of quality-assured suppliers around the world, to establishing centralized international procurement. Focusing on ensuring access to existing drugs, both for current needs and pandemic preparedness, might not make for scintillating television, but may improve the outcome of the next real-life pandemic.