Pandemic Preparedness Cannot Forget Existing Tools or Existing Diseases
A version of this article appears in Policy Options magazine.
The negotiation text of the World Health Organization’s (WHO) proposed Pandemic Treaty, released Oct 30th, contains language around not only equitable access to pandemic products like medicines and vaccines, but sustainable production of these products. Thankfully, Canadian proposals that would have undermined equitable access were not fully incorporated into this draft. However, throughout the development of this treaty, and of other recent international and domestic instruments to tackle pandemics, the discussion has consistently focused on novel tools for new and emerging pathogens. Sustainable production must be backward- as well as forward-looking; the global community cannot forget the ongoing need for access to existing tools necessary to combat old foes from past pandemics.
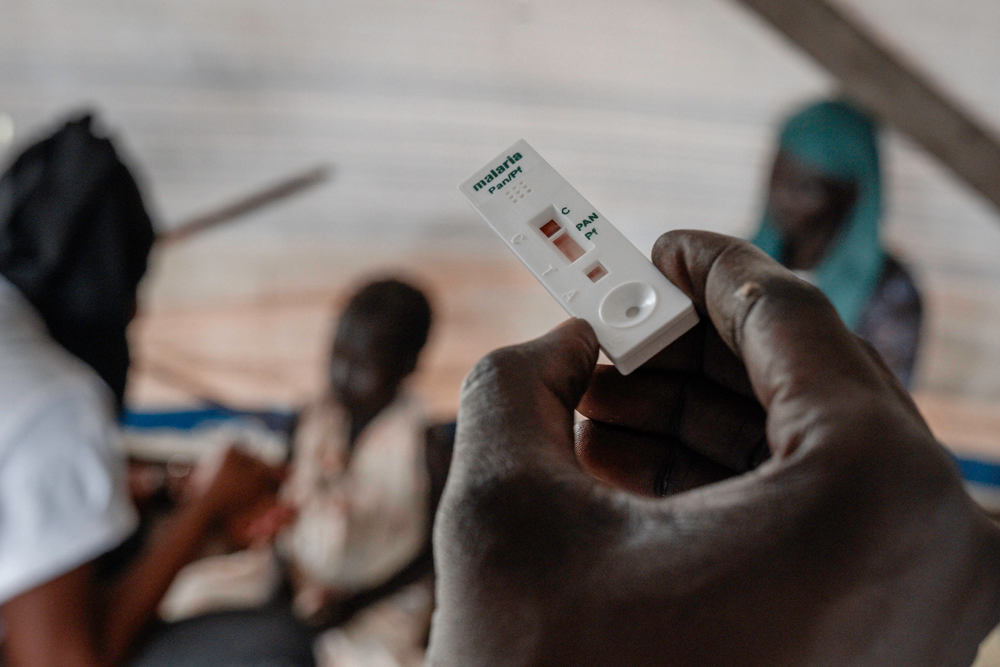
October also marked the one-year anniversary of the announcement that a global shortage of cholera vaccine had forced the International Coordinating Group (ICG) – the international body which manages emergency supplies of vaccines during major disease outbreaks, and whose members include the WHO and Doctors Without Borders/Médecins Sans Frontières (MSF) – to suspend the standard two-dose cholera vaccine regimen. Nevertheless, despite scaling back to a less effective one-dose regimen, the ICG-managed stockpile still ran out two months later. This severe shortage capped a major upsurge of cholera in 2022, with more than twice as many cases reported as the year before. Cases were reported in 44 countries, a 25 per cent increase from 2021; seven of these reported over 10,000 cases. In 2023, cholera, and access to cholera vaccine, has remained a serious concern.
It is particularly ironic that while COVID-19 vaccines have been the primary impetus for negotiating equitable access, cholera vaccines have attracted so little attention even amidst the current shortage. It was the multiple cholera pandemics of the 19th Century that first brought countries together to create the first multilateral legal instrument in response to infectious disease. Today’s International Health Regulations (IHRs), also currently undergoing revision, are the direct descendent of that first instrument specifically targeting cholera over 130 years ago. Cholera remains a deadly problem for too many people. And while ensuring equitable global access to new discoveries is vital, from vaccines for COVID-19 and RSV to monoclonal antibody therapies for Ebola and different cancers, so too is ensuring that longstanding tools remain available to those who still need them.
The shortage also illustrates how maintaining sustained access to existing tools has been a lower global priority. The key reason for the current shortage is that pharmaceutical companies don’t see cholera vaccines for outbreaks in lower-income countries as a sufficiently lucrative market. Indeed, a crucial element was the decision by Shantha Biotechnics, a subsidiary of pharmaceutical giant Sanofi and one of just two manufacturers of the cholera vaccine in the ICG-managed stockpile, to discontinue production at the end of 2022. While Sanofi provided advance notice of this discontinuation, other companies did not step in to fill the void in the market, and Sanofi didn’t call off discontinuation once the supply crisis became apparent.
Even as the stockpile’s remaining supplier, South Korea’s Eubiologics, increases production, and other sources belatedly emerge, global demand is still not being met. In May of 2023, Gavi, the Vaccine Alliance, made the grim prediction that the shortage would not be resolved until 2025.
This bears a moment of reflection. In December 2019, COVID-19 was a novel disease with no vaccine; within two years, not only had numerous effective vaccines been developed (sometimes pioneering novel technology), but over 8 billion doses had been administered worldwide (albeit inequitably). Compare this to the 120 million doses of cholera vaccine distributed in total from the ICG stockpile in the first decade since its founding in 2013. Clearly, manufacturing a far smaller amount of a pre-existing vaccine should be achievable in less time than it took to develop and roll out novel vaccines for a previously unknown disease; however, this requires adequate resources and attention. While there are provisions within the draft Pandemic Treaty regarding measures to assess global production and demand for pandemic-related products, as well as establishing and maintaining national, regional and international stockpiles, gaps remain when it comes to ensuring that crucial pre-existing products will be available to stock those stockpiles in the first place.
Yet even as the global stockpile for cholera outbreaks runs dry, some pharmaceutical companies still think they can make money selling cholera vaccines. Unfortunately, those plans don’t involve producing them for residents of cholera-prone countries. For instance, in February 2023, Bavarian Nordic announced it would acquire Vaxchora, a cholera vaccine for travelers approved in the United States and Europe, from Emergent Biosolutions. Bavarian Nordic is best known for its mpox vaccine, which is variously known as Imvamune/Jynneos/Imvanex in different high-income countries where it is available, including Canada, but has never been marketed in any of the African countries where mpox has been present for decades. In May 2023, less than a week before Gavi’s grim cholera vaccine forecast, Vaxchora was approved by Health Canada.
Unlike the vaccines distributed via the ICG, Vaxchora isn’t meant for populations regularly exposed to cholera. Vaxchora is intended to protect people exposed to cholera for the first time, such as travelers from high-income countries; a high-dose version for cholera-endemic countries has yet to emerge. The result is the disquieting scenario of a tourist from a rich country being able to get vaccinated before visiting a country facing a cholera outbreak, while that country’s citizens lack vaccines.
Cholera vaccine is far from the only tool that remains vital for global health, but has largely disappeared from the commercial marketplace as the diseases they combat fade from memory in high-income countries. Diphtheria antitoxin (DAT) is another example. Diphtheria was once a leading killer of Canadian children; in turn, Canada’s Connaught Laboratories, later famed for the discovery of insulin, were originally founded to produce an affordable, accessible supply of DAT. Today, even amidst serious outbreaks in 2023 in Nigeria and elsewhere, few suppliers of this lifesaving treatment remain anywhere. The implications of this lack of supply also manifest in high-income countries on those occasions when cases do occur locally. DAT is no longer formally sold in Canada; instead, different levels of government maintain stockpiles of imported, unapproved DAT in case of emergency. Meanwhile, lack of commercial interest means new tools for diphtheria treatment like monoclonal antibodies that could replace the cumbersome 19th Century methods still used to make DAT struggle to get from lab to patient. Yet even as Canada embarks on a domestic biomanufacturing strategy, sustaining access to old tools, and more broadly filling gaps for both old and new tools the commercial market ignores, is largely overlooked.
The global free market has failed cholera vaccines and other old but important products. This means states will need to act, and do so collectively, whether through employing sticks or carrots with private companies, or by treating public production of tools like cholera vaccine as a global public good. As the Canadian government oft said of COVID-19, it’s not over anywhere until it’s over everywhere. As long as old diseases like cholera linger, the world needs to collaborate to ensure the tools to respond remain available wherever, and for whomever, they are needed.