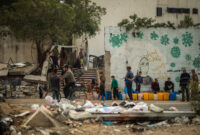Palestine: ‘For one year no one came here. It was a very difficult situation’
More than half of the West Bank is under Area C designation, meaning it is under direct Israeli civil and military control, which among other things translates into barriers to access healthcare for the approximately 300,000 Palestinians that live in small dispersed communities. More than one-third of them depend on mobile clinics to access essential health services.
Reaching the nearest clinic often entails costs that people cannot afford and travelling long distances with no public transportation and bad road conditions that prevent ambulances from being able to reach the communities in need. In cases requiring proximity to health services (e.g. pregnancy), there is also a need for them to stay away from home for a long period.
Masafer Yatta, in Hebron governorate, is an Area C zone where there have been virtually no medical services for a long time, as the national organiations providing mobile clinics suspended their activities for a variety of reasons, including funding cuts and stricter legislation impacting local NGOs. This has been exacerbated by the pressing needs of the healthcare system as a result of the COVID-19 pandemic.
MSF community-based support
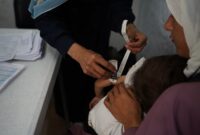
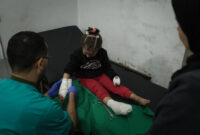
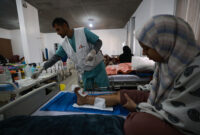
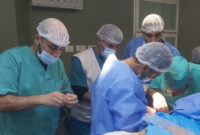
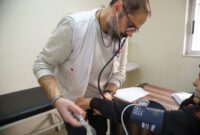
A few weeks ago, Doctors Without Borders/Médecins Sans Frontières (MSF) teams started visiting these communities again to provide basic healthcare, with a range of activities including general outpatient consultations (with a focus on children and patients with chronic communicable diseases), reproductive health, mental health and nutritional screening. Basic tests are also performed at these clinics and severe cases or those needing further testing are transferred to the nearest available hospital, in the town of Yatta.
Since November, MSF has been regularly visiting three areas – Dkaika, Djinba and Khirbet Al Fakheit – and in the last week a fourth one, Um Gussa, has been added. Our teams include a medical doctor, a nurse, a midwife, a mental health specialist and a health promoter. Almost 300 consultations have been performed since activities started.

“For one year, no one came here and our people had to go all the way to Yatta to get access to healthcare services,” explains Mohamad Ayoub Hamad, a community leader in Khirbet al Fakheit, where MSF teams perform mobile medical activities. “It was a very difficult situation especially for pregnant women. Put simply, families without a car really face a big problem,” he adds.
Centralized system leaves women out
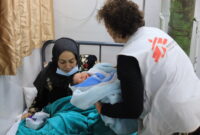
The women living in the area face in particular challenges accessing healthcare. Men regularly go to the nearest town, Yatta, to buy and sell products and they can seek health services there if needed. But the women usually work around the clock in the farmlands and, as they have no replacement, many tend to neglect their health and wait until their condition becomes serious before seeking medical attention. In addition, there is no public transport system in Masafer Yatta and, even if some families have a car, these are considered “illegal” as they are not registered and can be confiscated at any time.
Rasha[1] travelled to the mobile clinic in Khirbet Al Fakheit by donkey from her nearby village. “Things are completely different now. At least we have a doctor visiting us weekly and we can get medication. Before, if I needed any for myself or the kids, I would go around the village to all the houses to see if the neighbours had some,” she explains. The week before, Rasha had brought her two children for a check-up. In addition to all her problems, she says that “we are now short of money at this time of the year as we do not have cheese or buttermilk to sell.”
An additional hurdle for healthcare in this area is that the population in Area C is not allowed to build any permanent or semi-permanent structures without a permit from Israeli authorities, which is hardly ever granted. Even the humble structures used by MSF for the mobile clinics, like the one in Khirbet Al Fakheit, are mostly under threat of being knocked down. Since 2012, the school and the clinic next door have had a demolition order which means that they could be bulldozed any day.

“We hope that some national organizations or the Palestinian Ministry of Health will soon have the capacity and the funding to provide services again to the communities living in areas like Masafer Yatta,” says Katharina Lange, MSF’s Hebron project coordinator.
MSF in Palestine
MSF started working in the Palestine in 1989 focusing on delivering primary healthcare in Gaza. In 1996, mobile clinics started in some Hebron areas (C and H2) and a decade later the activities were handed over to another organisation. Besides the medical activities in Hebron, MSF currently runs mental health programmes in Hebron and Nablus, in the West Bank. In Gaza, MSF runs inpatient departments and clinics to treat patients with trauma and burns. We provide plastic and orthopaedic surgery to close large wounds and begin the process of repairing loss of and damage to the bone, as well as providing dressings, physiotherapy, health education and psychosocial support.
[1] Her name has been changed at her request to protect her anonimity
Related news

Palestine: MSF resumes core lifesaving activities at Nasser hospital

Middle East and North Africa: Behind the armour, men’s mental health

Palestine: Ceasefire in Gaza, humanitarian aid must flow immediately