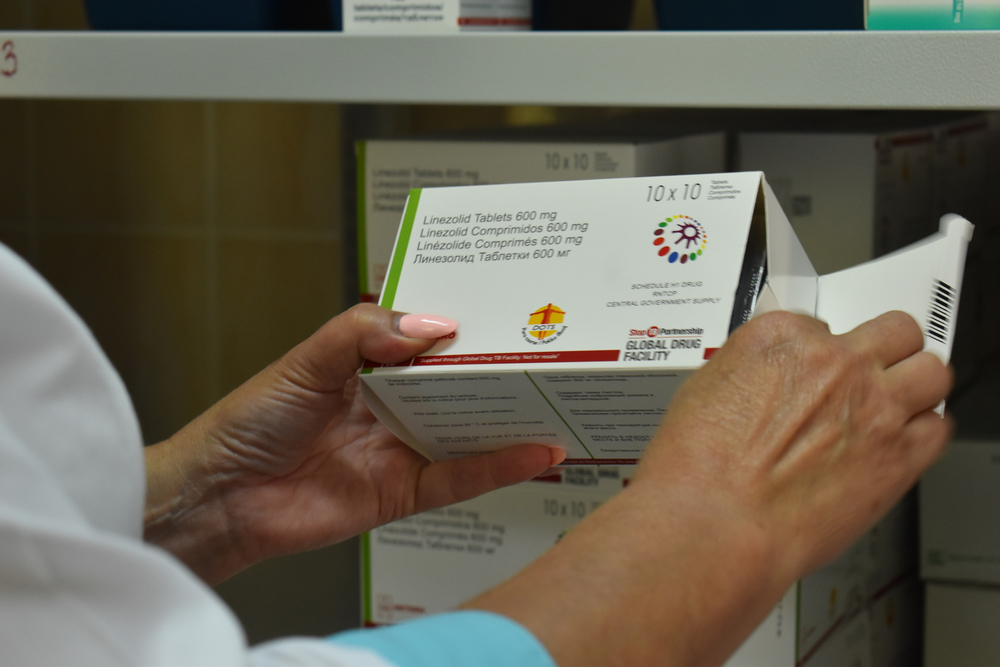
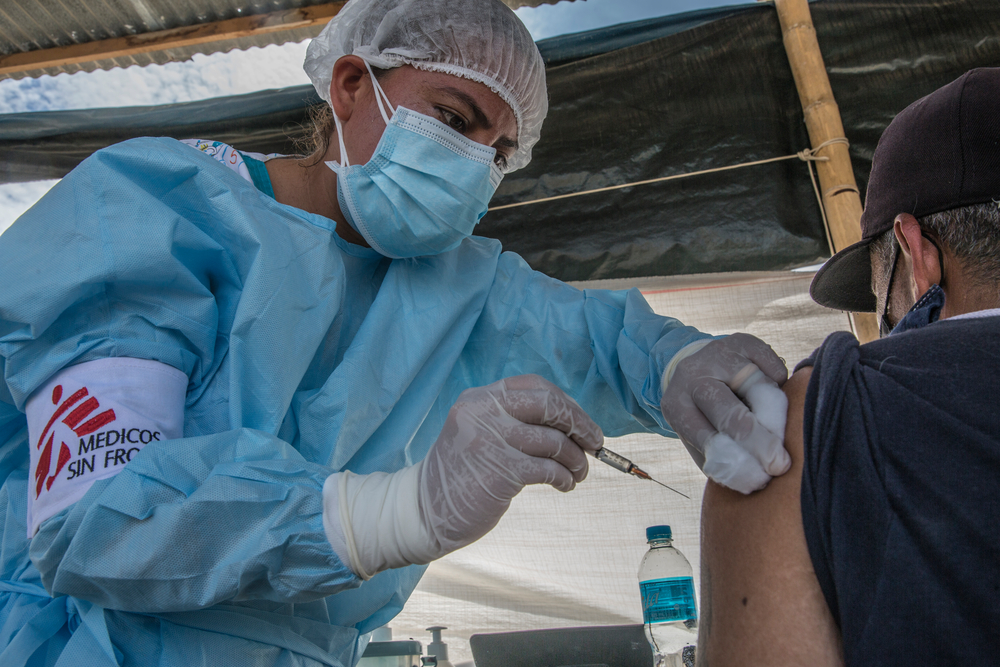
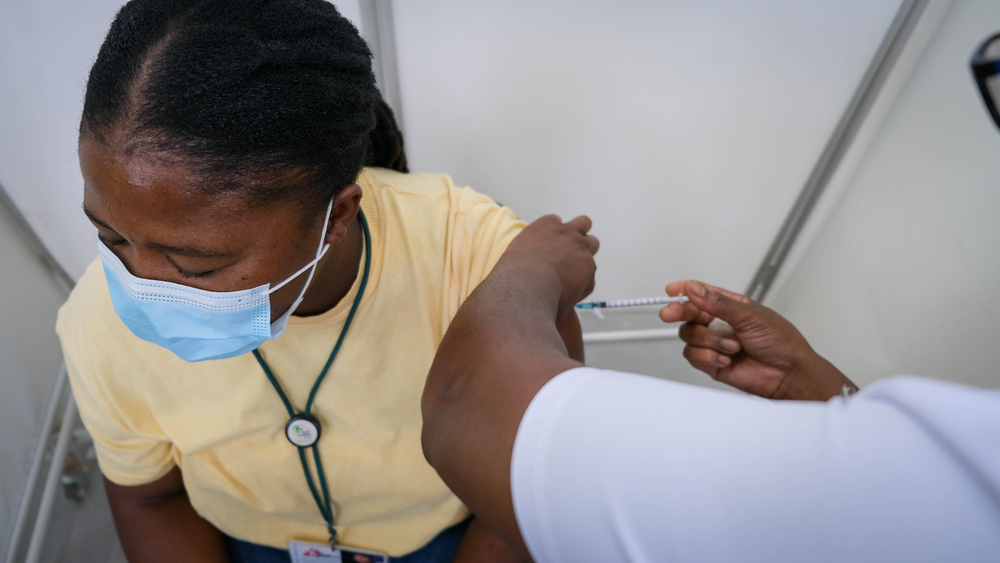
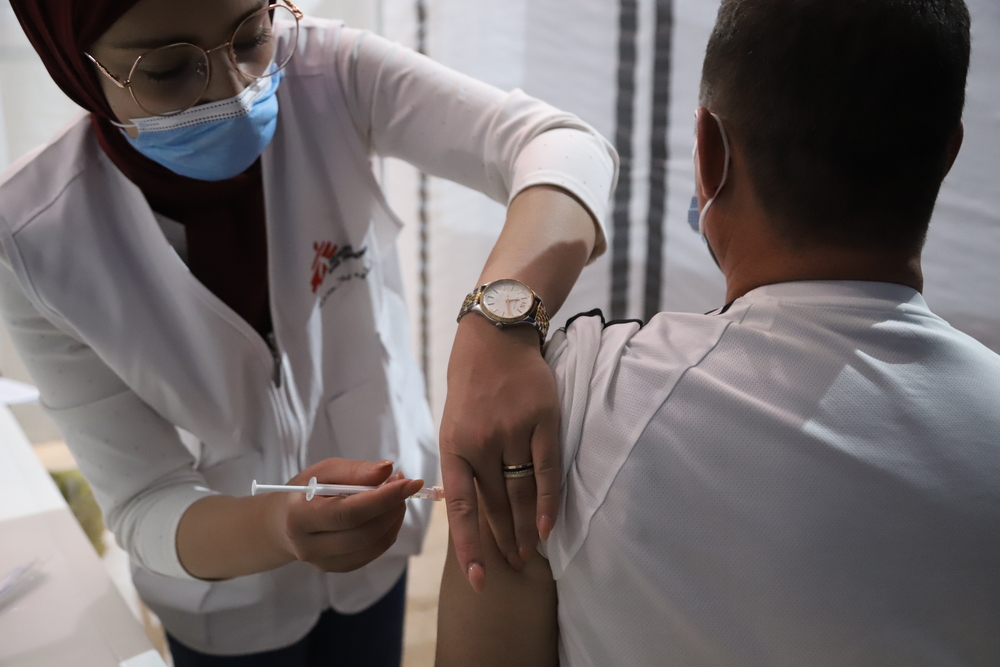
Governments must demand pharma make all COVID-19 vaccine licensing deals public
After the worrying terms of a deal struck between pharmaceutical corporation AstraZeneca and Brazilian public research body Fundação Oswaldo Cruz (Fiocruz) were disclosed recently, Doctors Without Borders/Médecins Sans Frontières (MSF) called on governments to urgently demand transparency from pharmaceutical corporations on all COVID-19 vaccine licensing agreements, as well as clinical trial costs and data, especially considering the billions of dollars of public, taxpayer money that have gone towards the development of these potential vaccines.
Fiocruz took an important step towards more transparency by publishing online the license agreement with AstraZeneca to produce at least 100 million vaccine doses (AZD1222) – although the agreement was published with redactions, it nonetheless represents a step that should encourage other governments to follow suit and take action towards more transparency.
A previous agreement showed that there are limits to AstraZeneca’s public ‘no profit’ commitments, and that the company has given itself the power to declare the pandemic over as soon as July 2021. This means that, after July 2021, AstraZeneca could charge governments and other purchasers high prices for a vaccine that was entirely funded by the public. The original exclusive license between AstraZeneca and Oxford University has still not been made public, the terms of which largely determine the terms of the company’s subsequent deals with other vaccine manufacturers around the world. People with knowledge of the AstraZeneca-Oxford license have questioned AstraZeneca’s ‘no profit’ commitment, saying that AstraZeneca may charge as much as 20% more than the costs associated with producing the vaccine. Other than the agreement with Fiocruz, sub-licenses with other manufacturers in South Africa, India and other countries, have also not yet been disclosed. Public scrutiny of the terms of these deals is critical to ensure equitable and affordable access to these future life-saving vaccines.
Traditional lack of tranparency
Pharmaceutical corporations have a very poor track record of transparency across the board – from licensing deals and technology transfers to costs of R&D and clinical trial data – and the little information that has been revealed around AstraZeneca’s not-for-profit promises should be a warning sign that pharma cannot be trusted to act in the interest of public health.
As long as we don’t know what’s in these deals, pharma will continue to hold the power to decide who gets access when, and at what price
Kate Elder | Msf Access Campaign Senior Vaccines Policy Advisor
TWEET THIS:
“As long as we don’t know what’s in these deals, pharma will continue to hold the power to decide who gets access when, and at what price,” said Kate Elder, Senior Vaccines Policy Advisor for MSF’s Access Campaign. “Without decisive action from governments demanding more transparency from companies, equitable access to COVID-19 vaccines is in jeopardy. The public has the right to know what’s in these deals – there is no place for secrets during a pandemic, there is too much at stake.”
Race for the COVID-19 vaccine
The licensing deals struck for a number of other companies racing to develop COVID-19 vaccines also remain cloaked in secrecy, despite unprecedented levels of public funding. Over US$12 billion has been poured into the research and development (R&D), clinical trials and manufacture of six front-runner candidate COVID-19 vaccines developed by AstraZeneca/Oxford University (over $1.7 billion) Johnson&Johnson/BiologicalE ($1.5 billion), Pfizer/BioNTech ($2.5 billion), GlaxoSmithKline/Sanofi Pasteur ($2.1 billion), Novavax/Serum Institute of India (nearly $2 billion), and Moderna/Lonza ($2.48 billion). AstraZeneca has gone so far as to state several times that the development of the vaccine will have no financial implications for the company since “expenses to progress the vaccine are anticipated to be offset by funding by governments and international organizations.”
Canada has also taken important steps to secure access to COVID-19 vaccines for people around the world, but has announced that it has signed agreements allowing for the purchase of up to 358 million doses of vaccines for use in Canada — enough to fully vaccinate every Canadian five times. “Given the urgent need to ensure that high risk people everywhere are protected against COVID-19, including healthcare workers, people living in refugee camps, and people living in places affected by conflicts and other emergencies, it’s essential that we understand how Canada will ensure that any excess doses of vaccine that it has purchased or supported the manufacture of, will be directed toward ensuring the kind of global, equitable access that Canadian leaders have promised,” said Dr. Jason Nickerson, MSF Canada’s Humanitarian Affairs Advisor.
Canada is not just a purchaser of vaccines, it’s also directly supporting the research and development of new COVID-19 vaccines, therapeutics, and other health technologies through more than $1-billion of public funding. “This funding ought to be provided with common-sense safeguards included to require that the recipients take reasonable steps to ensure the vaccines and medicines being developed with public funds are made affordable and accessible for patients, whether they be in Canada or any other country,” says Dr. Nickerson.
MSF recently delivered a petition signed by more than 90,000 people calling on the Canadian government to change the way it funds medical research and development to include safeguards that ensure medicines, vaccines, and other health technologies developed with public funds are affordable and accessible once they are developed.
MSF also urged COVID-19 vaccine developers to disclose clinical trial costs and data. Without this information, it is impossible for people, treatment providers and governments to demand affordable prices and scrutinize critical safety and efficacy data. Given that R&D and manufacturing costs have been largely – or entirely, in the case of AstraZeneca and Moderna – offset by public contributions, the public deserves to see a transparent breakdown of these costs and data.
“Despite repeated assurances from Heads of State that any COVID-19 vaccine will be a global public good, and despite claims that we’re seeing industry at its best, the reality is that up to this point it is clear that pharma cannot be trusted to act in the interest of public health, even in these unprecedented times,” said Roz Scourse, Policy Advisor for MSF’s Access Campaign. “Even with billions of dollars of public, taxpayer money paying for these vaccines, and billions of lives at stake, we continue to be left in the dark, leaving us scrambling to determine critical information such as the price and supply of any future COVID-19 vaccines, and what this means for equitable access.”
Governments must be bold at this critical juncture for the health of billions of people, take responsibility for the billions of public dollars that they have handed over for these vaccines, and demand that pharmaceutical corporations urgently make public all licenses, agreements, clinical trial costs and data related to COVID-19 vaccines.