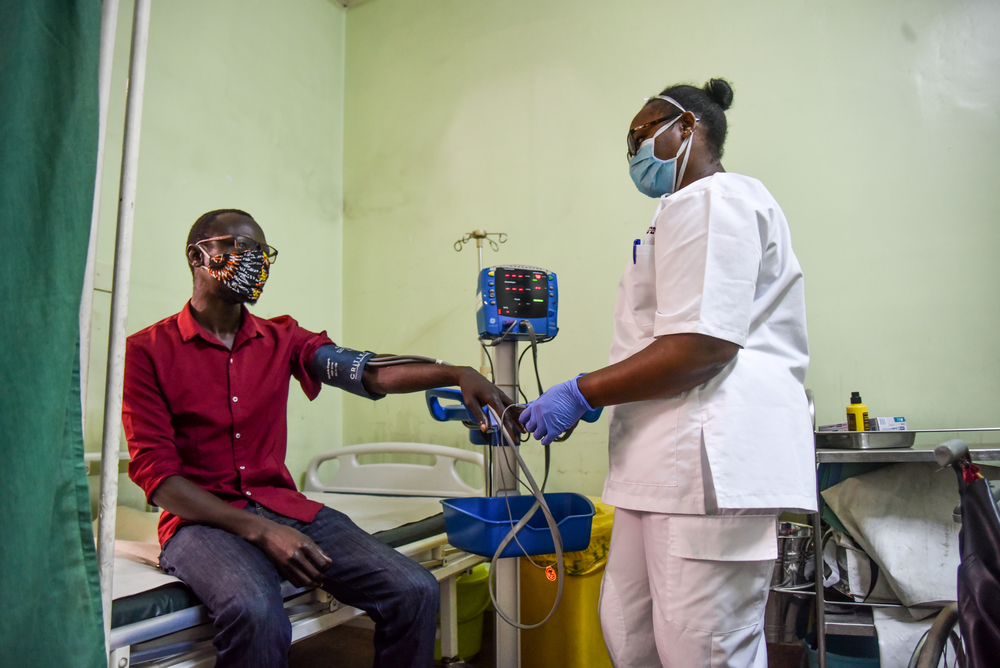World Tuberculosis Day 2020: COVID-19 and TB require global solidarity
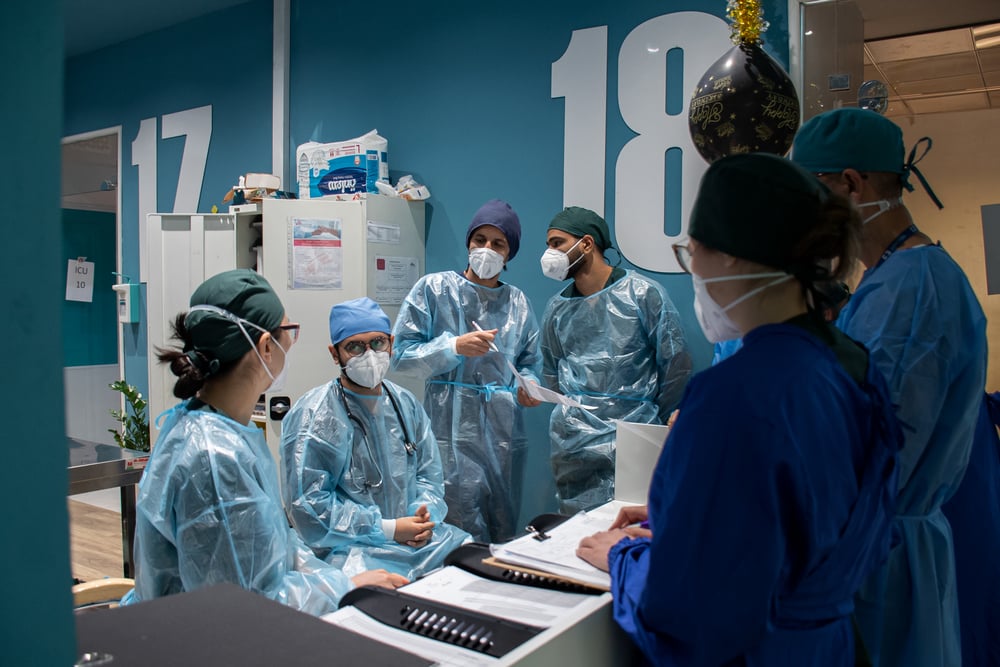
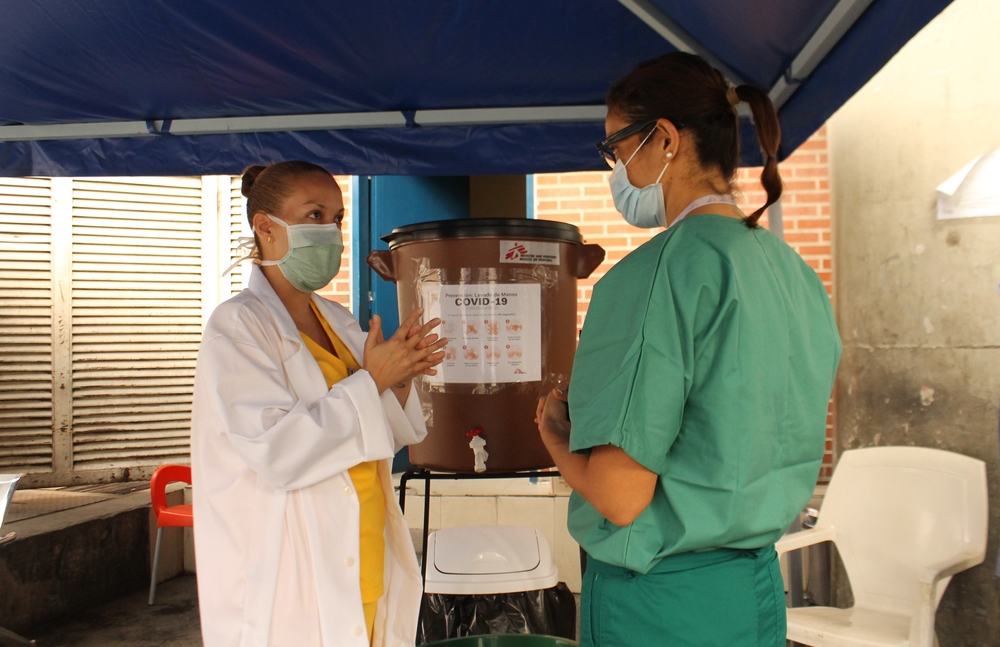
As the world grapples with the global pandemic of COVID-19, Doctors Without Borders/Medecins Sans Frontieres (MSF) is concerned for vulnerable groups worldwide. On World TB Day we wish to draw attention to people with tuberculosis (TB), as they are among the groups that may be doubly affected. Special attention will be needed to safeguard the continuity of prevention, diagnosis, treatment and care for people with TB worldwide.
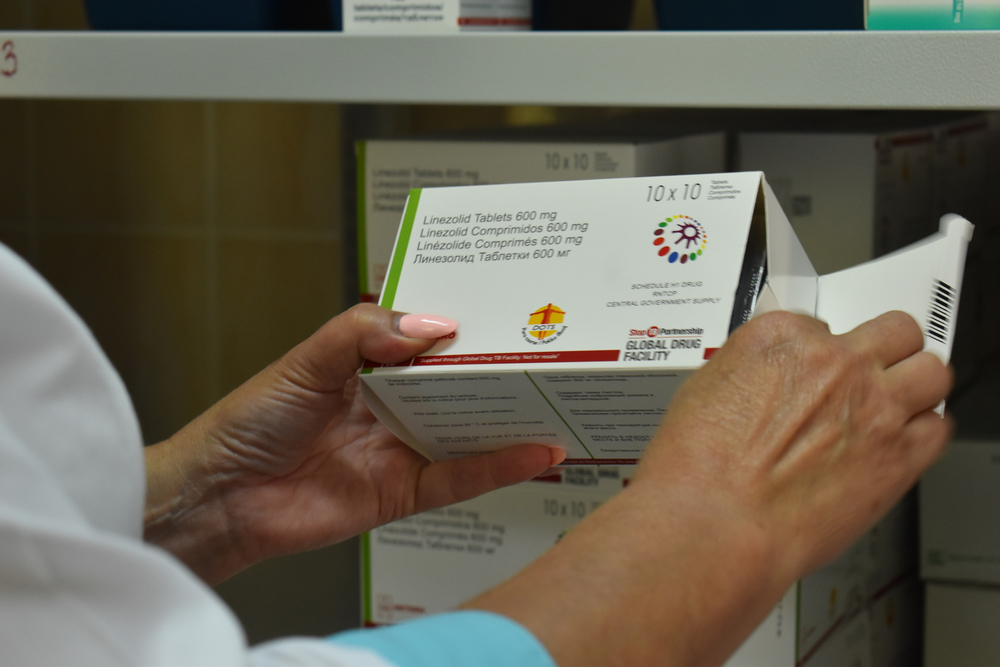
TB is the world’s leading infectious disease killer with nearly 10 million people affected and 1.5 million deaths in 2018. Half a million people have drug-resistant forms of TB for which the treatment is long and toxic. TB is also the leading cause of death among people living with HIV. Many countries – such as India and South Africa – have large numbers of people living with both HIV and TB.
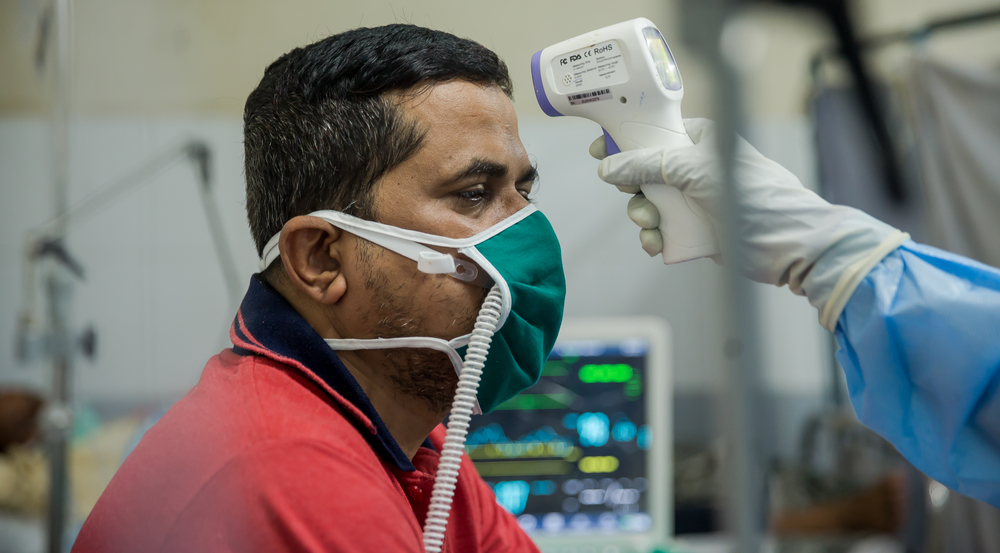
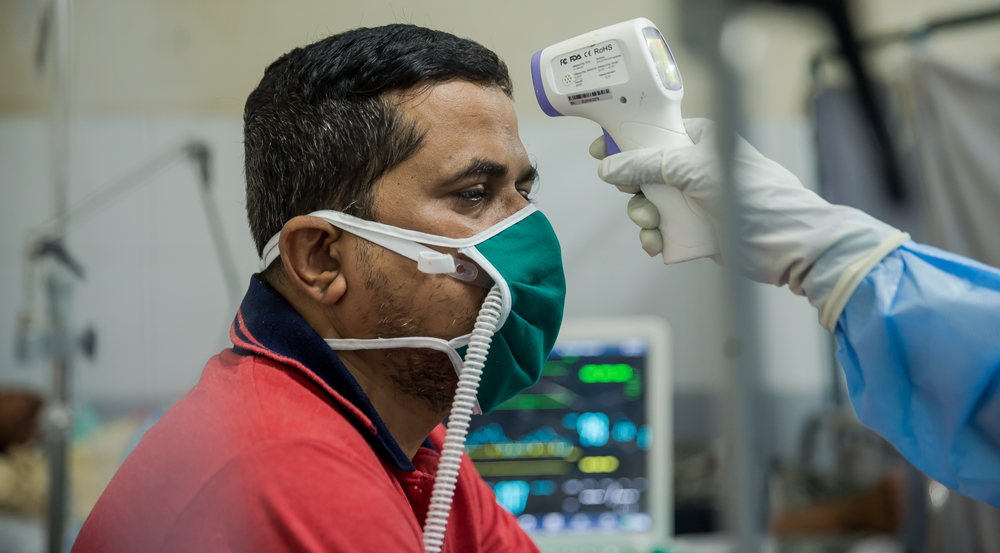
As with TB, COVID-19 typically affects the lungs and people who contract it may show similar symptoms to TB, such as coughing and fever. It’s likely that people with lung damage such as TB patients or those with weak immune systems such as those with poorly controlled HIV may suffer from more severe forms of COVID-19, if infected. In addition, many patients with TB live in densely populated areas, and this close proximity further increases their risk of getting COVID-19. In particular in overcrowded settlements with little access to clean water or healthcare.
COVID-19 pandemic could affect HIV & TB treatments
This already concerning situation will become even more grave if diagnosis and treatment for HIV or TB is interrupted. As such, MSF supports the World Health Organization’s (WHO) information note on strategies to maintain continuity of essential services – prevention, diagnosis, treatment and care – for people living with TB and drug-resistant TB (DR-TB) during the COVID-19 pandemic.
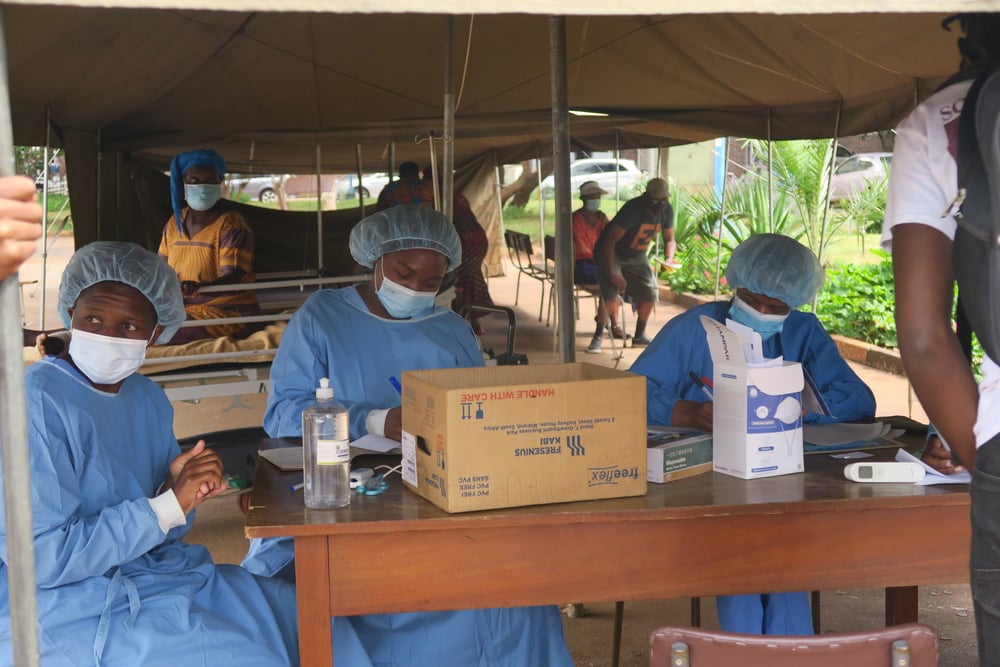
Health care systems particularly those in low resource settings will be put under considerable pressure by the COVID-19 virus. We know from previous epidemics that reduced access to care, medicines and diagnostics for people with life-threatening conditions, such as TB, can lead to an increase of deaths from these underlying conditions. In Guinea, one of the countries at the epicentre of the 2014-2015 Ebola epidemic, reduced health services led to a 53% decrease in the diagnosis of TB, and a doubling of the mortality rate from it from direct and indirect impacts on TB health services.
Concurrent to the global response needed to tackle COVID-19, health authorities, implementing partners, and international funders must make every effort to maintain essential services, while reducing the risks for vulnerable populations.
To reduce the risk of COVID-19 infection amongst TB and HIV patients, we will need to see innovative changes to the ways in which healthcare is provided: this includes decentralized and outpatient treatment, access to treatment through community and ‘physically distant’ models of care and follow up of patients through telemedicine and the use of web apps. The implementation of all oral treatments for drug resistant TB as recommended by WHO is now an imperative that cannot be delayed, as is the implementation of community supported treatment to reduce contact with health structures.
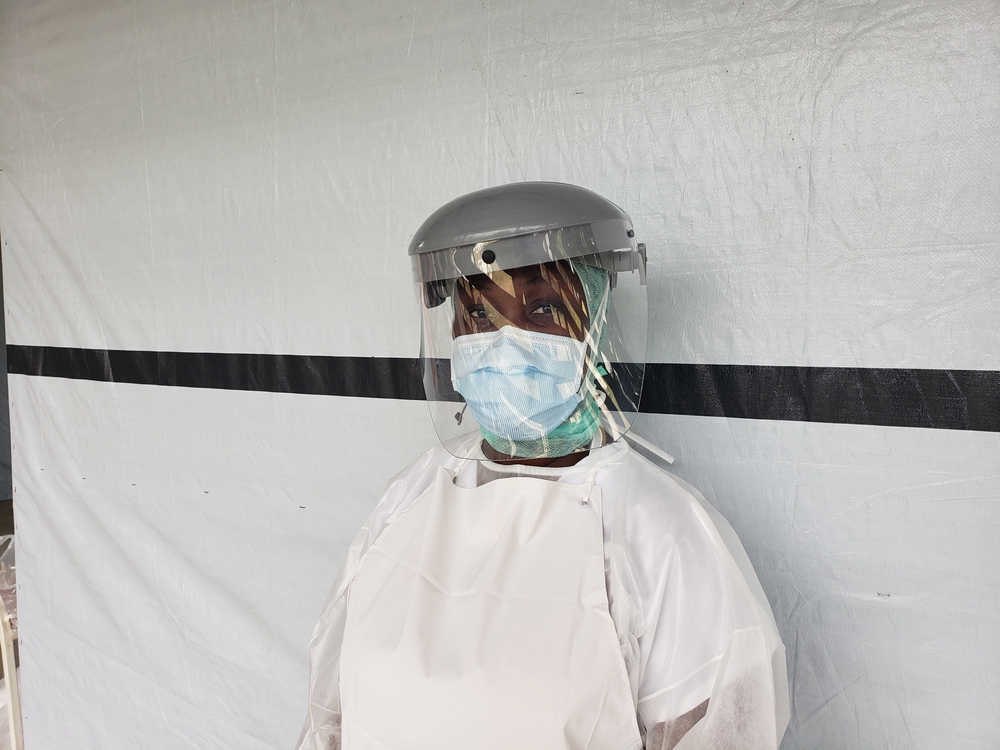
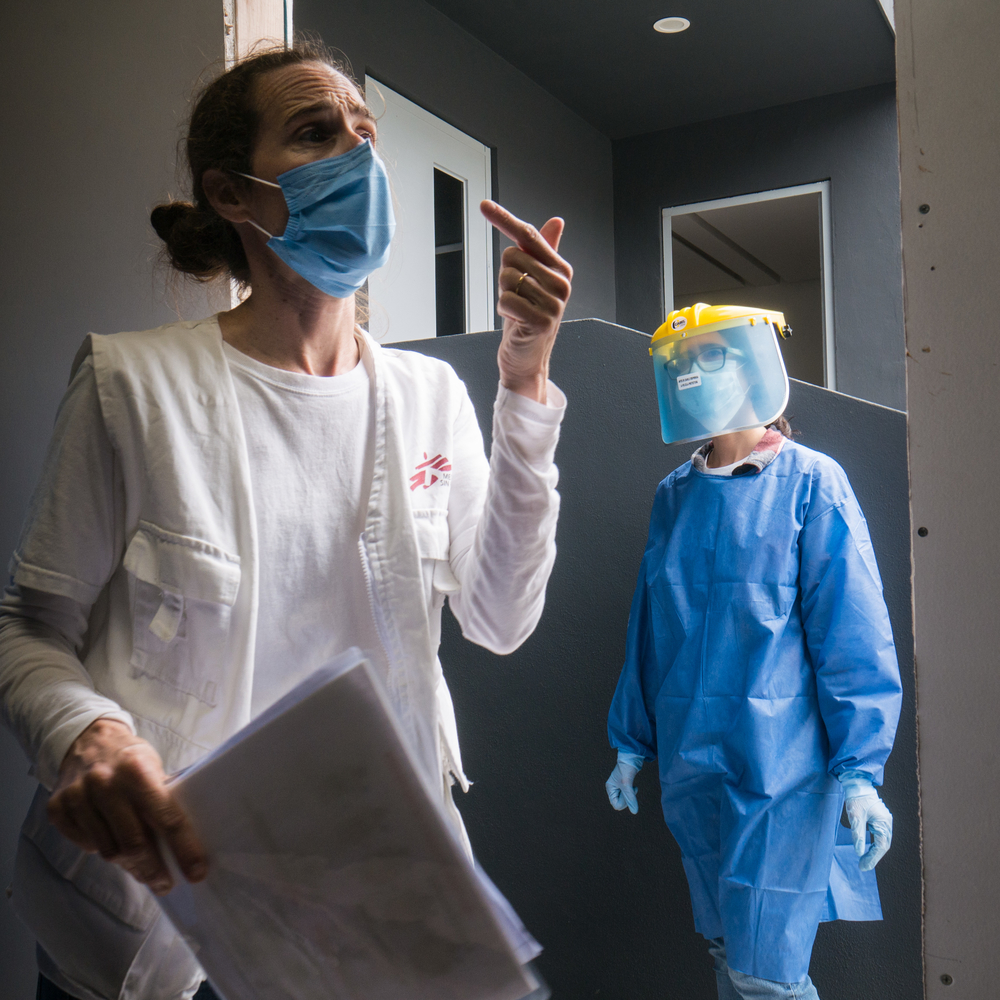
Given the high risk of severe disease in TB patients, efforts to minimize the impact of COVID-19 should also include the provision of protective measures for staff and those in contact with TB patients and the testing and isolation of confirmed or suspected COVID cases to avoid transmission to others.
Global solidarity is essential to tackling a global pandemic. Avoiding excessive stockpiling and export bans, will ensure essential medicines and supplies, including personal protective equipment, can reach all countries in need. Such collaboration and sharing will reduce the risk that people TB are put at additional risk because of lack of necessary drugs or ability to test. Without such an approach the pressure on countries with already fragile health systems will be doubled. As countries struggle to deal with COVID-19 pandemic, we must take all necessary steps to ensure that the impact of this pandemic does not create a second tragedy for vulnerable communities worldwide, including people with TB and HIV.